Top 5 Tips for Managing the Holidays

Top 5 Tips for Managing the Holidays: More Joy, Less Stress

- Plan Ahead. Last minute travel or outings can be difficult depending on the medical conditions and special needs in your family. If you’re flying for the holidays, call your airline ahead of time and ask about their policies for medical supplies (many airlines will allow a free additional carry-on for medical supplies). To lighten your luggage load, consider shipping certain supplies ahead of time. Most hotels will hold a package ahead of your arrival and Real Food Blends meals can be shipped to any destination in the United States — just make sure to call your hotel to ask what needs to be included on the shipping label so you’re sure to get your package.
- Always Be (Over) Prepared. Even if you’re not traveling for the holidays, odds are you’re going to be spending some extra time away from home this month (even if it’s just to run typical holiday errands). Pack a bag with extra supplies to have in your car just in case–extra syringes, Real Food Blends meals, buttons, extensions, pump bags, blender bottles, etc. You never know how long an outing might really take (especially when you factor in crowds or inclement weather) and you won’t have to rush as much if you know you have extra supplies on hand if you need to fit in an unexpected meal away from home.
- Manage Mealtime. If you or your loved one only recently got a feeding tube, or if you’re celebrating with friends
and relatives you don’t seeon a regular basis, this might be your loved ones’ first experience seeing a feeding tube. If possible, explain ahead of time how mealtime will work for you or your loved one — we always encourage including family members with feeding tubes during meals just like everyone else! Having a feeding tube isn’t something to be ashamed of — it’s just a different way of getting food into your stomach — so explain the process to loved ones with questions (and even offer for them to help if they want to). Our Turkey, Sweet Potatoes & Peaches meal is a great option during the holidays since it includes several common holiday foods and gives your loved one with a feeding tube another way to feel included during mealtime.
- Communicate Your Needs. Whether you need to leave a function early, have to duck out to give a medication, need a designated quiet room to use during the family get-together, or need some extra help getting all your holiday errands done, tell your loved ones what you need and what they can do to help. If that means that certain holiday activities just can’t happen this year, or need to change from previous years, that’s OK.
- Be Kind To Yourself. Even in ideal situations, the holidays can be stressful. No one gets to every single item on their “to do” list and no trip or event ever goes exactly as planned. Remember, it’s important to take care of yourself during the holidays, too, so take breaks when you can and treat yourself however you can. After all, what’s most important during the holidays is spending time with those you love, not seeing how many errands you can run, events you can attend, or chores you can get done around the house. Make sure to make time for your own joy and fun in the middle of all of your “to do’s.”
The Value of Daily Values

The Value of Daily Values?
What’s really behind all those nutrition numbers
by Sarah Kiser, MS, RD, CSO, CNSC
There are many terms to describe “nutrient needs.” DRIs, RDIs, RDAs, DRVs, ABC123s (just kidding on that last one), but what do they all mean? What do they mean for people with feeding tubes?
In the feeding tube world, the phrase “nutritionally complete” gets used a lot, but it’s important to know that formulas are made nutritionally complete with the use of supplements. (Read “The Facts About ‘Nutritionally Complete” here.) First, we need to get into some definitions. There are two general classes of analyzing nutrient needs: Daily Values (DVs) and Dietary Reference Intakes (DRIs). They overlap and are sometimes used interchangeably, but it is helpful to know where the differences lie.
Daily Values (DVs)
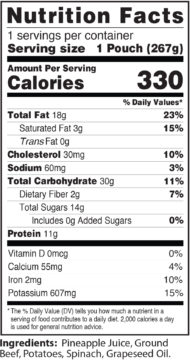
DVs are reference amounts of nutrients to consume. These are the percentages you see listed on the Nutrition Facts panel on food labels. DVs are based on two things:
- Reference Daily Intakes (RDIs): a set of references for vitamins and minerals on food labels based on recommended dietary allowances (RDAs)
- Daily Reference Values (DRVs): these are established for fat, saturated fat, cholesterol, carbohydrates, protein, dietary fiber, sodium, and potassium
RDIs typically represent the recommended nutrients of the group with the highest need. For example, the RDI for vitamin D is 20 mcg, which is the RDA for adults over the age of 70. Meanwhile, the RDI for calcium is 1300 mg, which is the RDA for children 9-18 years of age. These age groups have the highest need for vitamin D and calcium, respectively. That means the DV does not represent the much wider population which typically doesn’t need as much vitamin D and calcium. These reference values listed on food labels simply provide context for consumers to know what they are eating and are intended to cover the widest group of people possible.

DVs are:
- Used on food labels
- Provide perspective on daily nutrient needs for adults and children ages 4 and up
- Based on a 2,000-calorie diet
DVs are not:
- Recommended intakes for individuals
- Age, gender, or life stage specific
- Always applicable to those who need less or greater than 2,000 calories daily
Dietary Reference Intakes (DRIs)
In contrast to RDIs, DRIs do vary by age, gender, and life stage. DRIs are used to determine nutrient needs for healthy people. The most important terms to know related to DRIs are:
- Recommended Dietary Allowance (RDA): The average daily level of intake that meets the nutrient requirements of 97-98% of healthy people;
- Adequate Intake (AI): established when there isn’t enough data to create an RDA. This is set at a level assumed to ensure nutritional adequacy for healthy people.
RDAs are broken out by age and gender with predetermined heights and weights. These reference weight-and-height values are not necessarily ideal; they simply make it possible to define recommended nutrient intakes appropriate for the largest number of people. RDAs meet or exceed the actual requirements of all but 2-3% of the population. Some people may not meet RDAs with their daily diets but may still meet their individual requirements.
While DRIs are more age, gender, and life stage specific than DVs, DVs are used on food labels and many enteral formula labels. Remember, DVs only provide information on daily nutrient needs for people 4 years old and older and are not recommended intakes for individuals.
One thing that DVs and DRIs share in common? They are both created for healthy people. People with feeding tubes fall across the spectrum of “health” and often have more unique needs to consider. A child with failure to thrive or an adult with severe muscle wasting probably do not fall into the reference weight-for-height values used to determine RDAs.
DRIs and DVs are certainly useful in serving as a benchmark for nutrient needs. But for people with feeding tubes especially, it is important to remember that the DVs shown on many formula labels aren’t necessarily accurate for your specific needs. When determining nutrient needs for an individual person, it is important to consider that their specific medical diagnoses, medications, weight and weight changes, and symptoms of nutrient deficiencies.
Food or Supplements?
The Dietary Guidelines for Americans state that your nutritional needs should be primarily met through a variety of nutrient-dense foods across all food groups. The American Institute for Cancer Research recommends that most people aim to meet nutritional needs through a healthy, varied diet alone, and cautions against using dietary supplements to decrease cancer risk.
Supplements are not intended to substitute for food and cannot duplicate all of the benefits from whole foods. Beyond vitamins and minerals, whole foods contain thousands of important nutrients, like carotenoids, flavonoids, and other antioxidants and phytochemicals that are not found in supplements. Many of these nutrients work together to enhance absorption and reduce risk for chronic disease, and supplements do not replicate the synergistic effects of nutrients in real food.
The evidence supporting the benefits of multivitamin and nutrient supplements is mixed. While it may seem that dietary supplements are all innocuous, it is important to remember that this is not the case. For example, high-dose beta-carotene supplements have been linked to an increased risk for lung cancer in current and former smokers.
Some populations may benefit from vitamin and/or mineral supplements added to a whole food, varied diet. It is always recommended that you consult with your registered dietitian or physician to evaluate your individual nutrient and supplement needs, whether you eat through a feeding tube or mouth!
The bottom line is: food first, supplements second – if necessary.
What Does This All Mean for Tube-Feeding?
The Real Food Blends Difference
Real Food Blends is the only line of tube-feeding formula that truly replicates a whole food, varied diet that is universally recommended for good health – without added synthetic vitamins or minerals. Real Food Blends meals feature:
- Only 5-7 real food ingredients.
- No added sugar, preservatives, or additives.
- Free from gluten, soy, nuts, and dairy.
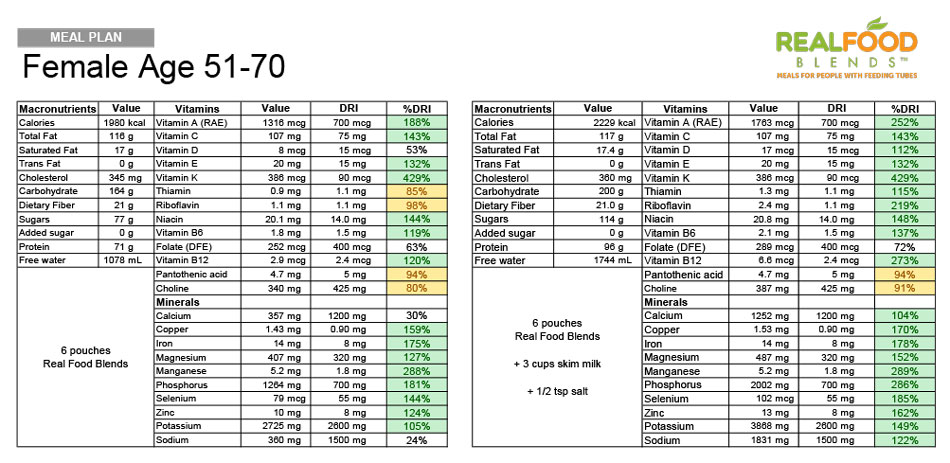
Check out how our meals compare to the DRIs for different age ranges without adding in synthetic vitamins or minerals. When used as a primary source of nutrition, we recommend adding dairy (pourable Kefir is one of our favorites for the Calcium and probiotics) or a non-dairy substitute to round out calcium and vitamin D intake, as well as a source of sodium, like salt or broth. Remember, individual needs may differ from the DVs and DRIs, but in general, most dietitians agree that it’s better to eat an orange than take a Vitamin C supplement and hitting these goals every day shouldn’t be at the expense of the basics of good nutrition (i.e. avoiding added sugars, processed foods, eating a wide variety of whole foods, etc.)
Sarah Kiser, MS, RD, CSO, CNSC is a Business Development Manager for Real Food Blends and has more than 6 years of experience as an oncology dietitian and working with home healthcare companies.
Getting Started with Real Food Blends

Getting Started With Real Food Blends
Tips for transitioning from formula
The information below is not medical advice. Always work with your medical team before making any changes to your enteral nutrition, especially if you have never consumed real food before or have reason to suspect allergies. Keep in mind that one Real Food Blends meal equals 8 ounces (one typical can of formula).
Seven day sample schedule for getting more out of real food

- The number of Real Food Blends pouches you will need per day will vary based on your daily caloric goal set by your medical team. Don’t be surprised if you need more calories from real food than you required on formula – this is common and luckily volume tolerance tends to increase with real food as well to help make hitting those goals easier!
- Whenever possible, we like to encourage working toward a normal mealtime schedule of breakfast, lunch, and dinner (with maybe a snack or two thrown in for extra calories), versus continuous or overnight feeds. If you have been on continuous feeds, it may take some time to get toward this schedule, but often this can be done once the body adjusts to having real food again.
- We like to encourage the use of the slow-push bolus feeding method with a syringe to keep our meals as thick as possible. The thickness tends to help with reflux symptoms and can provide a feeling of satisfaction that a pure liquid meal doesn’t always provide. When you are transitioning, though, you might find it easier to mix the meals with some formula or water for a thinner consistency or to feed through a pump or gravity bag. That’s okay! The point is to start getting some real food into the body and you can slowly head toward bolus feeding when ready.
- After day 7, ideally you would introduce the other two RFB varieties into your diet and continue to rotate the meals. For even more variety, consider some simple additions like whole milk or pourable Kefir for added calcium. Our Real Food Blends recipe book has more ideas too!
How to Use Real Food Blends
Adding to Real Food Blends Meals
Additional Tips
- Add water to meet hydration needs – same as oral eaters do! Discuss with your medical team about how much water is needed and also take note of outputs. In general, urine should be pale yellow and stools easy to pass. Additional water may be necessary in hot weather and/or when ill.
- RFB meals contain no added sodium. If you’re not on a sodium restricted diet, adding anywhere from ¼ to 1 teaspoon of salt per day would meet your daily sodium requirements (depending on your age and weight). Always consult with your medical team on exact needs.
- RFB meals contain no added synthetic vitamins or minerals. You may want to consider adding an age-appropriate multi-vitamin along with a calcium supplement to meet your nutritional needs once fully transitioned to RFB.
- If a thinner consistency is required, add water/fluid to the pouch via syringe. Warming can also help thin the meals if desired.
- Knead the meal before opening the package to improve consistency, especially if the meal has been exposed to colder temperatures.
How to Administer Real Food Blends Using Bolus Method
Step 1: Open Pouch

Step 2: Insert Syringe & Draw

Step 3: Slow Push to Administer

Interested in trying Real Food Blends for the first time? Our Trial 6-Pack is a great place to start as it has one of each of our five meals!
Feeding Tube Tips for Heading Back to School

Feeding Tube Tips for Heading Back to School
The start of a new school year is an exciting time for all families, but sending your child with a feeding tube to school for the first time can be nerve-wracking for both parents and kids. That’s why we put together our tips for tube feeding at school, particularly when using our meals or a home blended diet. With a little preparation and organization, tube feeding at school doesn’t have to be that different from feeding at home.
Before School Starts
Most schools will require a doctor’s note or doctor instructions to feed your child during the school day. Including your child’s feeding plan in their IEP and 504 plans is also important. Offer to train the person who will be feeding your child at school, whether that is the school nurse, an aide, or someone else. Also make sure at least two people are trained to feed your child in case the main person is ever unavailable. The Feeding Tube Awareness Foundation has a free School Training Presentation designed to train school nurses, teachers, aides, and other school staff about tube feeding. Be specific about volume and feeding times in the feeding schedule you have on file with the school. If your child uses a pump, tell school staff how to deal with any pump alarms that might happen. Many schools will have a specific protocol for how they handle a feeding tube that comes out during the school day, so make sure you know your specific school’s policy, including if you can send an emergency kit to replace a feeding tube at school.

Preparing for the First Day
Ahead of your child’s first day of school, make sure you label everything you’re sending, from syringes to insulated bags to pump bags and backpacks (if used). If your child is using Real Food Blends meals, you can send them to school without an ice pack or cooler, but make sure the school is aware that any leftovers need to be refrigerated within 2 hours of opening the pouch. If the school allows you to send food ahead of time, you can send Real Food Blends meals one week at a time or more since they are shelf stable for 3 years from the date of manufacturing. If you bolus feed and are sending blends from home, or just want to save time during the school day, mom Kara recommends sending prefilled syringes. “I prefill syringes and cap them for the nurse daily. Then I put them in a one-gallon Ziplock bag with a primed extension. Makes it easier for the nurse and in turn a quicker experience for our son!” Just remember with this option, whether you’re using home blends or Real Food Blends, to send the pre-filled syringes in a cooler/insulated bag with ice packs and make sure the syringes are refrigerated at school until they are ready to be used.
Helping Your Student Adjust
While you may be nervous about sending your child to school for the first time with a feeding tube, remember that your child might be nervous, too! If this is your child’s first overall experience at school, they may have questions about their new schedule and who will be helping them throughout the day. Make sure to walk your child through their schedule and explain to them where they need to go for tube feedings and who will be helping them. Don’t be afraid to adjust your child’s feeding schedule during the school year, too. Being nervous about a new routine might mean your child won’t be able to take the same volume at school—consider making lunch smaller and incorporating a before or after lunch snack into their school feeding schedule or an after school snack at home. When possible, we always encourage those using Real Food Blends to use a mealtime schedule just like those who eat orally, which often includes a snack in addition to breakfast, lunch, and dinner. We’re just talking about food, after all!
If your child previously ate orally, they may be nervous about answering questions about their feeding tube at school and how lunchtime will be different. Giving a presentation to your child’s class about tube feeding at the beginning of the school year can be a great way to alleviate some of these worries for your child and make his or her classmates feel more at ease with feeding tubes. Feeding Raya has a great example of a presentation her kids gave to their classes about their younger sister with a feeding tube. For preschool or kindergarten classes, reading My Belly Has Two Buttons to the class is a great option as well.
If anyone at your child’s school has questions about Real Food Blends, our new RD Hub is a great resource or you’re welcome to direct them to call us at 888-484-9495. You can also reach out to us via our Facebook page. The Feeding Tube Awareness Foundation also has a wealth of general tube feeding information, especially for those new to tube feeding. From all of us at Real Food Blends, we wish you and your child a fantastic school year!
The Story Behind Our Meals

The Story Behind Our Meals
Clean Ingredients, Clean Labels
Whether you’re new to Real Food Blends or have been using (or recommending) our meals for years, you may not know why our meals are the way they are. Although we started with three meals and now have six, we’ve stayed with the same philosophy from the beginning—that simple variety is best. If you’re an RD, you may recognize that our meals are based on the USDA’s Choose Your Plate guidelines and each includes a fruit, vegetable, whole grain, and protein; you only need to add a side of dairy to have a government-approved meal.
Meals, Not a Formula
What that means is that we have 5-7 ingredients in each of our meals on purpose—we believe whole food ingredients are best (the less processed, the better.) There’s no need to spend hours combing over our ingredient list to see if there’s something hidden in there that might interact with a medication or that might be a different form of an ingredient you or your loved one can’t tolerate—our ingredient lists will always be short, simple, and easy to read because we ONLY include real food ingredients in our meals.

When choosing the specific ingredients, we always include a full serving of fruits and vegetables in every meal along with a whole grain, lean protein, and healthy fat. Sounds a lot like what most doctors and dietitians recommend to their oral eating patients, right?! As long as the digestive system is still intact, what we all know about good nutrition still applies to those with feeding tubes. Does a vegetable become less good-for-you if it goes through a feeding tube? People with feeding tubes can benefit from healthy, real foods just like oral eaters—they just need a different way of getting those foods into their stomachs. All of our ingredients are consciously sourced as well, including:
- Grass-fed beef
- Wild-caught salmon from the Pacific Northwest
- Only US-raised chicken and eggs
- Certified Gluten-free oats*
That being said, our ingredients are not organic, and that was also something we chose on purpose. We understand that organic is very important to some people, but we made the decision to focus on real, whole foods while keeping costs down so that our meals are affordable for people paying out of pocket and to make sure our meals are easily available to those with insurance coverage. The high heat process that our meals go through to make them shelf stable (which is the same process many food products go through to make them shelf stable) also can minimize any benefits that might be gained from using organic ingredients. Studies in general have been mixed as to the actual levels of increased nutrients in organic foods and many experts agree that WHAT you eat is more important than whether you choose organic versus conventional. If organic is important to you, we would highly encourage you to work with your dietitian and blend fresh organic food versus any organic tube-feeding formula that’s shelf-stable.
Why 6?
So now you know why we have simple, consciously-sourced, whole food ingredients in all six of our meals, but you might not know WHY we have six different meals. After all, in the past formulas for feeding tubes have been designed to have someone use the same formula all day, every day. That just didn’t make sense to us. People who don’t have a feeding tube are told to eat a wide variety of healthy foods every day, so why shouldn’t people with feeding tubes be given the same recommendations? Here’s what Alissa Rumsey, MS, RD, CDN, CSCS, a clinical dietitian at one of New York’s largest hospitals, has to say about that.
“Think about people who eat by mouth. No one eats the same meal and ingredients over and over again, every single meal, every single day. As a dietitian, I would never recommend that, even if the patient was taking a multi-vitamin every day. So why are we recommending it to people on tube feeds? Nutritional variety is just as important –if not moreso- as nutritionally complete.”
What’s NOT In There
Now that we’ve talked about what IS in our meals, what about what ISN’T? Like added synthetic vitamins. We know some medical professionals focus on nutritionally complete products for their enteral patients (read more about the concept of nutritionally complete), but we kept added synthetic vitamins and minerals out of our meals for a variety of reasons.
- Synthetic vitamins can cause nausea and leave a nasty after-taste when burped.
- Not all people with a feeding tube need the same amounts of these vitamins, given their underlying conditions. It’s not unusual for someone to need a low-sodium diet, low potassium, or have other unique nutritional needs that are not one-size-fits-all.
- Potential for medication interactions.
- Potential to greatly exceed RDIs.
After all, once you put vitamins in, you can’t take them out. Everyone has individual nutrition needs, different medications that can impact certain vitamin and mineral levels, and different health considerations. A child with cystic fibrosis isn’t going to have the same nutritional needs as an adult who suffered a traumatic brain injury. Consult your medical team for your specific nutritional needs, but in general, if you’re using our meals as a sole source of nutrition, we just recommend adding a daily multivitamin and a dash of salt once a day (our meals have no added salt, either!).

We hope this sheds some light on the story behind the creation of our meals, especially for those who are newer to Real Food Blends. No matter what, know that our meals will always contain nothing but simple, whole food ingredients that provide real food and nutritional variety for people with feeding tubes. Our co-founders, Tony and Julie Bombacino, founded Real Food Blends after seeing their own tube-fed son improve so drastically on a blended diet—we will always only offer meals that we’re proud of and contain ingredients we would feed our own families.
Interested in trying Real Food Blends for the first time? Our Trial 6-Pack is a great place to start as it has one of each of our five meals!
*Our meals are not certified as gluten free, but do not contain any gluten ingredients. They are produced in a gluten handling facility.



 on a regular basis, this might be your loved ones’ first experience seeing a feeding tube. If possible, explain ahead of time how mealtime will work for you or your loved one — we always encourage including family members with feeding tubes during meals just like everyone else! Having a feeding tube isn’t something to be ashamed of — it’s just a different way of getting food into your stomach — so explain the process to loved ones with questions (and even offer for them to help if they want to). Our
on a regular basis, this might be your loved ones’ first experience seeing a feeding tube. If possible, explain ahead of time how mealtime will work for you or your loved one — we always encourage including family members with feeding tubes during meals just like everyone else! Having a feeding tube isn’t something to be ashamed of — it’s just a different way of getting food into your stomach — so explain the process to loved ones with questions (and even offer for them to help if they want to). Our